
Health Care Professions Merit Badge — Complete Digital Resource Guide
https://merit-badge.university/merit-badges/health-care-professions/guide/
Introduction & Overview
A worried family member, a crowded waiting room, a paramedic radioing ahead from an ambulance, a lab tech checking a sample, and a therapist helping someone walk again all belong to the same huge team. Health care is not one job. It is a network of skilled people who keep patients safe, solve problems, explain confusing information, and help people recover.
This merit badge gives you a tour of that team. You will compare careers, visit a real workplace, think about medical ethics, learn why privacy matters, and serve your community. By the end, you should have a much clearer picture of where you might fit in the world of health care.
Then and Now
Then
For most of human history, medical care was local, simple, and limited. A village healer, midwife, barber-surgeon, or family doctor might be the only option. Tools were basic. Infection control was poor. Many treatments that seem obvious today — washing hands before surgery, using X-rays to see broken bones, giving insulin for diabetes, or replacing a damaged joint — did not exist yet.
As science improved, health care became more specialized. Doctors began focusing on areas like bones, eyes, or mental health. Nurses took on more formal training. Laboratories, pharmacies, hospitals, and medical schools became more organized. A patient with one illness might now be cared for by a whole team instead of just one person.
- Big change: medicine shifted from a mostly individual craft to a science-based team effort
- Why it mattered: better knowledge, better tools, and better training led to safer care and longer lives
Now
Today, health care combines science, technology, communication, and human compassion. A patient may see a nurse practitioner for a checkup, get blood drawn by a phlebotomist, have scans performed by an imaging technologist, receive medicine from a pharmacist, and work with a physical therapist during recovery. Electronic records help teams share information quickly, while strict privacy laws help protect that information.
Modern health care also moves far beyond hospitals. Care happens in clinics, schools, ambulances, rehabilitation centers, nursing homes, pharmacies, public health departments, sports facilities, and community events like vaccine clinics or blood drives. Some professionals work directly with patients every day. Others help by building devices, analyzing lab results, managing records, or improving systems behind the scenes.
- Big change: health care now depends on many specialized careers working together
- Why it matters today: patients need safe, accurate, respectful care from the first phone call to full recovery
Get Ready!
You do not need to know your future career right now. You just need curiosity, a willingness to ask good questions, and respect for the people who care for others every day. This badge is your chance to look behind the exam-room door and see how many paths exist.
Kinds of Health Care Professions
Health care careers can be grouped in a few big categories. These categories overlap, but they make it easier to understand what different professionals actually do.
Diagnosing and Leading Care
These professionals figure out what is wrong, decide on treatment plans, and guide the overall care of a patient. Physicians, nurse practitioners, physician assistants, podiatrists, psychologists, optometrists, and audiologists all fit here, even though they focus on different systems of the body or mind.
They need strong observation skills, careful judgment, and the ability to explain complicated ideas in plain language. A good diagnosis is not just a smart guess. It comes from listening closely, asking the right questions, gathering evidence, and choosing the next best step.

Bedside and Emergency Care
These professionals spend a lot of time directly with patients. Registered nurses, licensed practical nurses, nursing assistants, nurse midwives, nurse anesthetists, EMTs, and paramedics all help keep people safe when care must happen quickly or continuously.
They often notice changes before anyone else because they are close to the patient. They also bring calm to stressful moments. In many settings, they are the people a patient sees most often.
Rehabilitation and Daily Living Support
Some health care jobs focus on helping people rebuild strength, independence, communication, and confidence after an injury, illness, or disability. Physical therapists, occupational therapists, respiratory therapists, speech-language pathologists, dietitians, and orthotists/prosthetists are all part of this world.
Their work can be dramatic, like helping someone learn to walk with a prosthetic leg, or quiet and steady, like teaching exercises that slowly improve breathing or swallowing. Success is often measured in everyday wins: climbing stairs, buttoning a shirt, speaking more clearly, or returning to sports.
Testing, Imaging, and Technology
A huge part of health care happens behind the scenes. Medical technologists, phlebotomists, sonographers, radiology technologists, histotechnologists, cytopathologists, biomedical engineers, and medical records specialists help gather and manage the information that other clinicians need.
These jobs demand accuracy. One mislabeled blood sample, blurry image, or incomplete record can affect patient care. If you enjoy science, machines, computers, or solving technical problems, this side of health care may be especially interesting.
Public Health and Community Service
Not every health care job treats one patient at a time. Some professionals work to improve the health of entire communities through education, prevention, screenings, vaccination drives, and volunteer events.
This matters because good health care starts before a person becomes seriously sick. Teaching people how to stay healthy, spotting problems early, and helping communities get access to care are all part of the mission.
Now that you have a map of the field, you can start comparing real jobs and the training each one requires.
Req 1 — Diagnosing, Hearing, and Whole-Person Care
Select three of the professions from Group 1 listed below which interest you, then complete the following:
Group 1:
- Allopathic physician (MD)—all specialties
- Osteopathic physician (DO)—all specialties
- Podiatrist (DPM)
- Chiropractor (DC)
- Nurse Practitioner (NP)
- Psychologist (PhD or PsyD)
- Optometrist (OD)
- Audiologist (AudD)
This first career group is about diagnosing problems, guiding treatment, and helping patients understand what is happening to their bodies and minds. Some of these professionals work from the top down, looking at the whole person. Others focus deeply on one body system, such as the feet, eyes, or hearing. As you read, start narrowing the list to three careers that genuinely interest you.
For this page, focus on two things:
- what each professional actually does during a normal day
- how long the education and licensing path usually takes
Requirement 1a: Roles in Health Care
An ear infection, blurred vision, anxiety, foot pain, or a yearly physical can all send a patient to a different kind of professional. The role of each person depends on what problem needs to be solved and what kind of training that professional has.
Broad-Care Clinicians
Allopathic physicians (MDs) and osteopathic physicians (DOs) are fully licensed physicians. They diagnose illnesses, order tests, prescribe treatments, and may perform procedures or surgery depending on their specialty. Family doctors, pediatricians, cardiologists, and surgeons can all hold either degree.
The main difference is educational tradition. DO programs add extra training in whole-person care and the musculoskeletal system, but in daily practice MDs and DOs both work throughout modern medicine. For a Scout, the key point is simple: both are physicians who can lead patient care.
Nurse practitioners (NPs) are advanced practice registered nurses who can evaluate patients, diagnose common conditions, order tests, prescribe medicines in most states, and often serve as primary care providers. They usually combine strong nursing experience with advanced graduate education.
Specialists Focused on a Specific Area
Podiatrists (DPMs) focus on the feet, ankles, and lower legs. They treat injuries, deformities, diabetic foot problems, sports injuries, and long-term pain. If a person has trouble walking, a podiatrist may help prevent a small problem from becoming a major one.
Optometrists (ODs) examine eyes and vision. They test how clearly you see, prescribe glasses or contacts, look for signs of eye disease, and sometimes spot larger health problems such as diabetes or high blood pressure during an eye exam.
Audiologists (AudD) study hearing and balance. They test hearing, help fit hearing aids or other devices, and work with patients who have dizziness, ringing in the ears, or hearing loss. Their work can make school, conversation, and daily life much easier for patients.
Professionals Who Focus on Mind, Spine, or Function
Psychologists (PhD or PsyD) evaluate thoughts, emotions, and behavior. They may provide therapy, perform assessments, and help patients manage conditions such as anxiety, depression, trauma, or learning differences. They do not usually prescribe medicine unless they work in a special state or federal system with additional authority.
Chiropractors (DCs) focus on the spine, joints, muscles, and nervous system, especially how body structure may affect movement and pain. They often work with patients who have back pain, neck pain, posture issues, or certain sports injuries.
Choosing Your Three Careers
Pick jobs that show real differences- Include variety: Choose three roles that are not too similar. For example, a psychologist, an audiologist, and a podiatrist will give you a broader comparison than three kinds of physicians.
- Think about patient contact: Do you prefer careers with long conversations, quick diagnostic visits, hands-on treatment, or technical testing?
- Notice the setting: Some jobs are common in clinics, some in hospitals, and some in private practice offices.
- Ask what problem they solve: Every career exists because patients need a specific kind of help.
Requirement 1b: Education and Licensing
Many Scouts are surprised by how different the training paths can be. Two jobs might both involve direct patient care, but one may require a doctoral degree while another requires a master’s degree plus national certification. The point of this requirement is not to memorize every exam name. It is to understand the level of education, supervised training, and licensing each career requires.
A Simple Way to Compare Training Paths
Use these four questions for each career you choose:
- What degree is required?
- How many years of school does that usually mean after high school?
- Is supervised clinical training required?
- What license, board exam, or certification allows that person to practice?
Typical Patterns in Group 1
- MD / DO: bachelor’s degree, four years of medical school, then residency training in a specialty, plus national board exams and a state medical license
- DPM: bachelor’s degree, podiatric medical school, residency, board exams, and state licensure
- DC: undergraduate prerequisites plus chiropractic doctoral training, clinical experience, board exams, and state licensure
- NP: registered nurse preparation, then graduate-level advanced practice education, national certification, and state advanced practice licensure
- Psychologist: doctoral training in psychology, supervised clinical hours or internship, licensing exam, and state licensure
- OD: undergraduate preparation plus four years of optometry school, national board exams, and state licensure
- AudD: doctoral training in audiology, supervised clinical experience, exam or certification steps depending on state, and state licensure
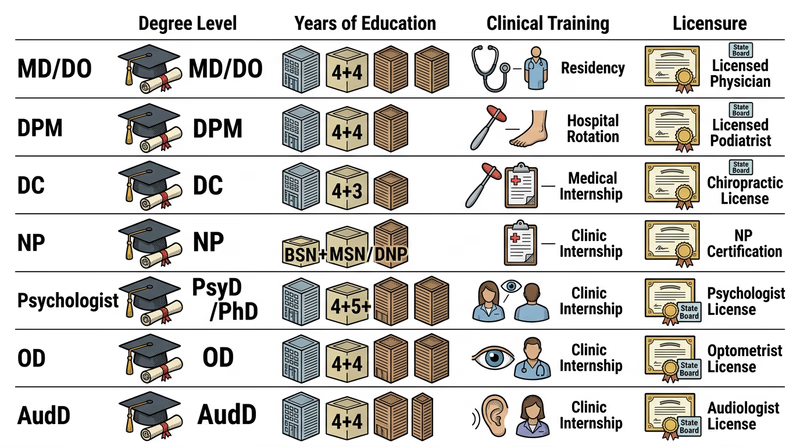
Why Licensing Matters
A license is the public’s safety check. It shows that a professional met minimum standards and is legally allowed to practice. Continuing education matters too. Health care changes fast, so professionals usually must keep learning to renew a license or certification.
A Strong Counselor Discussion
A good discussion compares careers, not just lists facts. You might say that an NP and a physician can both diagnose and treat patients, but their educational paths differ. Or you might compare an optometrist and an audiologist as two doctoral-level specialists who focus on different senses.
That kind of comparison shows that you understand how the health care team is built.
U.S. Bureau of Labor Statistics — Healthcare Occupations Career summaries showing what many health care professionals do, where they work, and the typical education needed. Link: U.S. Bureau of Labor Statistics — Healthcare Occupations — https://www.bls.gov/ooh/healthcare/home.htm AAMC — Careers in Medicine Profiles of physician specialties that can help you understand how broad the physician career path really is. Link: AAMC — Careers in Medicine — https://www.aamc.org/cim/explore-options/specialty-profiles American Academy of Audiology — What Is an Audiologist? An overview of what audiologists do and how they help patients with hearing and balance. Link: American Academy of Audiology — What Is an Audiologist? — https://www.audiology.org/consumers-and-patients/what-is-an-audiologist/In Req 2, you will compare another set of careers where direct bedside care, medicines, and emergency response are central to the job.
Req 2 — Bedside Care and Fast Decisions
Select three of the professions from Group 2 listed below which interest you, then complete the following:
Group 2:
- Physician Assistant (PA)
- Registered Nurse (RN)
- Certified Nurse Midwife (CNM)
- Certified Nurse Assistant (CNA)
- Licensed Practical Nurse (LPN/LVN)
- Nurse Anesthetist (CRNA)
- Pharmacist (PharmD)
- Pharmacy Technician
- Emergency Medical Technician (EMT)/Paramedic
This group is about care that happens up close and in real time. These professionals give medicines, watch for changes, comfort patients, support births, respond to emergencies, and keep treatment moving safely. If Group 1 was about diagnosis and specialty expertise, Group 2 shows how much health care depends on people who are present, practical, and ready to act.
To make sense of this list, think about three themes:
- continuous patient care
- medicine and treatment support
- rapid response in urgent situations
Requirement 2a: Roles in Health Care
A hospital room at 2 a.m., an ambulance at a car crash, a pharmacy counter, and a delivery room all depend on different people doing the right job at the right time. Group 2 careers often involve close patient contact, strong teamwork, and fast decision-making.
Nursing Roles
Registered nurses (RNs) assess patients, give medications, monitor symptoms, educate families, and coordinate care. They work almost everywhere: hospitals, clinics, schools, public health agencies, camps, and home health settings. They are often the professionals who notice first when a patient is improving or getting worse.
Licensed practical nurses (LPNs/LVNs) provide basic nursing care under the direction of RNs or physicians. They may check vital signs, help with daily care, collect information, and give certain medicines depending on the setting and local rules.
Certified nursing assistants (CNAs) help patients with daily activities such as bathing, dressing, eating, and moving safely. They spend a lot of time near patients, which means they play an important role in comfort, dignity, and observing changes.
Certified nurse midwives (CNMs) care for patients during pregnancy, labor, birth, and reproductive health visits. They combine medical knowledge with coaching and support during one of the biggest moments in a family’s life.
Nurse anesthetists (CRNAs) help patients stay safe and pain-free during surgery or procedures by planning and giving anesthesia and closely monitoring breathing, heart rate, and other vital signs.
Medical and Medication Support
Physician assistants (PAs), now often called physician associates in some places, examine patients, diagnose illness, order tests, prescribe medicines, and help create treatment plans. They work in collaboration with physicians but often handle many patient visits on their own.
Pharmacists (PharmD) are experts in medicines. They check for safe dosages, watch for drug interactions, counsel patients on how to take medications, and sometimes give vaccines. Their job is not just handing over a bottle. It is making sure the medicine helps more than it harms.
Pharmacy technicians support pharmacists by preparing prescriptions, managing inventory, and helping the pharmacy run smoothly. Accuracy is critical because a mistake in medicine strength, labeling, or patient information can be dangerous.
Emergency Response
EMTs and paramedics care for patients before they reach a hospital. They assess the scene, protect the airway, control bleeding, support breathing, monitor vital signs, and transport patients safely. Paramedics usually have broader training and can perform more advanced procedures than EMTs.

Questions to Ask About Group 2 Careers
These questions can help you compare your three choices- How much patient contact is there? A CNA may be with patients for much of the day, while a pharmacist may split time between patient counseling and medication review.
- How fast are decisions made? EMTs and paramedics may decide in seconds. Some pharmacy and clinic roles allow more time to verify details.
- What kind of teamwork is required? Nearly all of these jobs depend on close coordination with others.
- What kind of stress is common? Some roles involve emergencies, some involve shift work, and some demand intense attention to detail.
Requirement 2b: Education and Licensing
Group 2 is a great reminder that “health care job” does not mean one standard training path. Some careers begin with a certificate program. Others require doctoral education. Some professionals must renew national certifications and complete continuing education every few years.
Common Training Patterns
- PA: bachelor’s degree, graduate PA program, national certifying exam, and state licensure
- RN: nursing degree, clinical training, national licensing exam, and state licensure
- CNM: registered nurse preparation, advanced graduate nursing education, national certification, and state advanced practice licensure
- CNA: short training program plus state competency evaluation or certification steps
- LPN/LVN: practical nursing program plus national licensing exam and state licensure
- CRNA: registered nurse preparation, critical care experience, doctoral-level nurse anesthesia program, national certification, and state advanced practice licensure
- PharmD: undergraduate prerequisites plus pharmacy school, licensing exams, and state pharmacist licensure
- Pharmacy technician: training program or on-the-job training depending on state and employer, plus certification or registration requirements in many places
- EMT / Paramedic: approved training program, cognitive and practical testing, state licensure or certification, and continuing education
Why Clinical Experience Matters
Health care cannot be learned from textbooks alone. These professions require hands-on supervised practice. A nursing student learns how to assess a real patient. An EMT trainee practices lifting, airway care, and patient transport. A pharmacy student completes rotations in real settings. That supervised experience helps turn information into judgment.
A Useful Comparison Strategy
When you prepare for your counselor discussion, compare careers by how quickly a person can enter the field and how much independence the job allows. A CNA or EMT can often begin much sooner than a CRNA or pharmacist. That does not make one career better than another. It simply shows how different roles fit different training levels and responsibilities.
American Nurses Association — What Is Nursing? A clear overview of the role nurses play in patient care and the many settings where they work. Link: American Nurses Association — What Is Nursing? — https://www.nursingworld.org/practice-policy/workforce/what-is-nursing/ MedlinePlus — Medicines: Using Them Safely Reliable patient-friendly information about medications, side effects, and safe medicine use. Link: MedlinePlus — Medicines: Using Them Safely — https://medlineplus.gov/medicines.html EMS.gov Information about emergency medical services, including how EMTs and paramedics fit into emergency care systems. Link: EMS.gov — https://www.ems.gov/In Req 3, you will shift from urgent and bedside care to careers that help patients recover skills, adapt, and regain independence over time.
Req 3 — Recovery, Communication, and Movement
Select three of the professions from Group 3 listed below which interest you, then complete the following:
Group 3:
- Physical Therapist (DPT)
- Occupational Therapist (OT)
- Orthotist/Prosthetist
- Medical Appliance Technician
- Respiratory Therapist (RT)
- Medical Assistant
- Dietitian (RD)
- Speech-Language Pathologist (Speech Therapist) (SLP)
A patient may leave the emergency room alive but still need months of work to get back to normal life. That is where Group 3 careers stand out. These professionals help people move, breathe, eat, communicate, use adaptive equipment, and manage everyday tasks after illness, injury, or disability.
This page is about care that often happens step by step. Progress may be slow, but it can be life-changing.
Requirement 3a: Roles in Health Care
Learning to walk again after surgery, using a new prosthetic leg, speaking clearly after a stroke, or managing asthma treatments at home all require different kinds of help. Group 3 professionals often work with patients repeatedly over time, which means they build strong relationships and celebrate many small wins.
Movement and Function
Physical therapists (DPTs) help patients improve strength, balance, flexibility, and movement. They guide exercises, measure progress, and design recovery plans after injuries, surgeries, or neurological conditions.
Occupational therapists (OTs) help patients do the activities of daily life. That can include getting dressed, writing, using kitchen tools, returning to school, or adapting a bedroom so a person can move more safely.
Orthotists/prosthetists design, fit, and adjust braces and artificial limbs. Their work combines anatomy, biomechanics, and careful listening because a device has to fit the person’s body and life.
Medical appliance technicians build, adjust, or repair certain devices and supports used in patient care. Depending on the setting, that may include orthotic or prosthetic parts, specialized equipment, or other custom medical aids.
Breathing, Nutrition, and Communication
Respiratory therapists (RTs) help patients breathe more effectively. They may manage oxygen therapy, breathing treatments, ventilators, and education for patients with asthma, pneumonia, premature birth complications, or chronic lung disease.
Dietitians (RDs) use food and nutrition science to help patients stay healthy or recover. They may work with people who have diabetes, food allergies, eating disorders, sports nutrition needs, or digestive conditions.
Speech-language pathologists (SLPs) help with speech, language, voice, swallowing, and communication challenges. Despite the name, their work goes far beyond pronunciation.
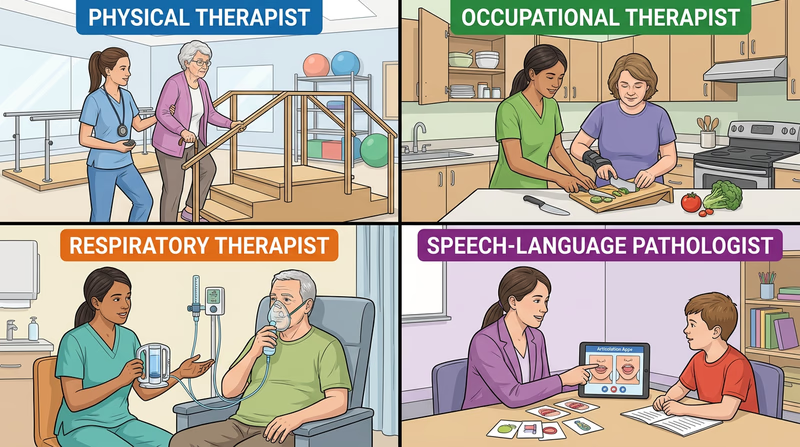
Clinic Support
Medical assistants support physicians and clinics by taking histories, checking vital signs, preparing rooms, managing records, and sometimes handling basic clinical tasks. They keep a practice organized and help patients move through visits smoothly.
What Makes Group 3 Different?
Look for these patterns as you compare careers- Longer recovery relationships: Many patients see these professionals repeatedly over weeks or months.
- Practical goals: Success may mean climbing stairs, breathing easier, swallowing safely, or returning to school sports.
- Adaptation matters: Equipment, exercises, and environment changes are often part of the solution.
- Teamwork stays important: These professionals often coordinate with physicians, nurses, families, and schools.
Requirement 3b: Education and Licensing
Training in this group ranges from certificate-level programs to doctoral degrees. A good comparison should show not only how much school each career requires, but also how much patient evaluation, planning, and independence the job includes.
Typical Training Patterns
- DPT: bachelor’s preparation, doctoral physical therapy program, national licensure exam, and state licensure
- OT: graduate occupational therapy education, fieldwork, national certification exam, and state licensure
- Orthotist/prosthetist: college-level preparation plus specialized graduate or certificate training, supervised residency, certification, and often licensure depending on state
- Medical appliance technician: program or technical training depending on role and employer, plus hands-on skill development
- RT: associate or bachelor’s level respiratory therapy education, clinical training, certification exams, and state licensure where required
- Medical assistant: certificate or diploma program, sometimes associate degree, and optional or employer-preferred certification
- RD: college degree, supervised practice, national exam, and in many states licensure or certification
- SLP: bachelor’s degree plus graduate speech-language pathology program, supervised fellowship, national exam, and state licensure
Matching Training to Responsibility
If a job includes diagnosis, independent treatment planning, or complex decision-making, the training path is usually longer. That helps explain why a medical assistant may enter the field more quickly than an SLP, and why a DPT usually trains longer than a respiratory therapist.
Questions Worth Asking
If you meet someone from one of these careers, ask:
- What kind of patients do you see most often?
- What skills took the longest to learn?
- How do you measure patient progress?
- What kind of schooling surprised you the most?
Those questions move the conversation past job titles and into real understanding.
American Physical Therapy Association — Choose PT An overview of what physical therapists do and how they help patients recover movement and function. Link: American Physical Therapy Association — Choose PT — https://www.choosept.com/ American Occupational Therapy Association — About Occupational Therapy A plain-language explanation of how occupational therapists help people participate in everyday life. Link: American Occupational Therapy Association — About Occupational Therapy — https://www.aota.org/about/for-the-public American Speech-Language-Hearing Association — Speech-Language Pathologists A patient-friendly overview of speech-language pathology and the communication and swallowing challenges SLPs address. Link: American Speech-Language-Hearing Association — Speech-Language Pathologists — https://www.asha.org/public/who-are-speech-language-pathologists/In Req 4, you will look at another side of health care: the professionals who test samples, capture images, manage records, and build the technology that supports diagnosis and treatment.
Req 4 — Testing, Imaging, and Behind-the-Scenes Care
Select three of the professions from Group 4 listed below which interest you, then complete the following:
Group 4:
- Biomedical Engineer (BME)
- Medical Technologist
- Phlebotomist
- Radiology Technologist
- Sonographer
- Medical Records Specialist
- Cytopathologist
- Histotechnologist
Some of the most important people in health care are not the ones a patient remembers by name. They are the people who draw the blood sample, prepare tissue slides, run the lab test, capture the image, protect the medical record, or design the machine that everyone else depends on. Group 4 shows how modern medicine relies on precision, data, and technology.
These careers are a great fit for Scouts who like science, computers, machines, organization, or solving technical puzzles.
Requirement 4a: Roles in Health Care
A doctor may suspect pneumonia, a tumor, anemia, or internal bleeding. But to move from suspicion to evidence, the care team often needs help from specialists in testing, imaging, and records.
Lab and Sample Specialists
Medical technologists perform and interpret many of the laboratory procedures that help detect disease. They analyze blood, urine, and other specimens to look for infection, chemical imbalances, blood disorders, and more.
Phlebotomists collect blood samples safely, label them correctly, and help keep the testing process moving. Their work may look simple from the outside, but it requires skill, calm communication, and careful identification.
Histotechnologists prepare tissue samples so they can be examined under a microscope. They cut thin sections, stain them, and make sure the specimen is ready for accurate analysis.
Cytopathologists are physicians or highly specialized experts who study cells to help diagnose disease, including certain cancers and infections.
Imaging and Visualization
Radiology technologists produce images such as X-rays that help clinicians see bones, lungs, and other internal structures. They must position patients carefully and follow safety procedures around radiation.
Sonographers use ultrasound equipment to create images using sound waves instead of radiation. They may help visualize organs, blood flow, or a developing baby during pregnancy.
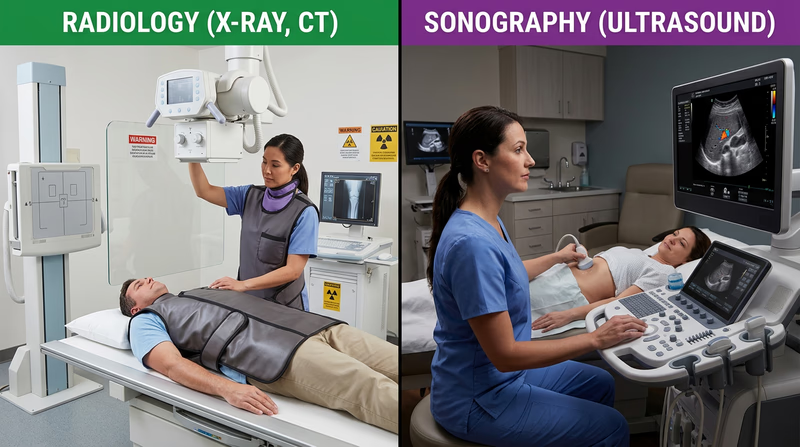
Information and Device Support
Medical records specialists manage health information so that records are accurate, organized, secure, and available to the right people when needed. Good records help prevent errors and support continuity of care.
Biomedical engineers (BMEs) design, improve, and sometimes maintain medical devices, systems, and technologies. That can include imaging equipment, prosthetics, monitors, surgical tools, and software that supports patient care.
How Group 4 Supports the Care Team
Think of these roles as evidence builders- They gather information: blood tests, tissue slides, imaging studies, and records all help answer medical questions.
- They improve accuracy: treatment decisions are stronger when the data is reliable.
- They work behind the scenes: patients may not interact with them for long, but their impact can be huge.
- They demand precision: a mislabeled tube or incorrect image can affect the next step in care.
Requirement 4b: Education and Licensing
This group includes one of the widest training ranges in the badge. Some careers start with technical programs or associate degrees. Others require physician-level or engineering-level education.
Typical Training Patterns
- BME: bachelor’s degree in biomedical engineering or related engineering field, with some roles requiring graduate study
- Medical technologist: college-level laboratory science education, clinical training, and often certification
- Phlebotomist: training program plus certification or employer/state requirements depending on location
- Radiology technologist: imaging program, clinical training, certification exam, and licensure in many states
- Sonographer: accredited diagnostic medical sonography program, clinical training, and certification in common practice
- Medical records specialist: certificate, associate, or bachelor’s preparation depending on role, plus coding or health information certifications for some positions
- Cytopathologist: physician education pathway plus advanced pathology training and board certification
- Histotechnologist: laboratory science education plus specialized histology training and certification
Why Accuracy Shapes Training
Even when the training path is shorter, the standards are still high. A phlebotomist may spend less time in school than a biomedical engineer, but both must master procedures that affect patient safety. The difference is not whether the work matters. The difference is the kind of knowledge needed for the role.
A Smart Way to Compare Careers Here
For each career you choose, ask whether the job is mainly about:
- collecting information
- analyzing information
- protecting information
- building the tools used to collect or analyze information
That question helps you explain the role clearly to your counselor.
Society of Diagnostic Medical Sonography — What Is a Sonographer? A career overview explaining what sonographers do and how ultrasound helps diagnose medical problems. Link: Society of Diagnostic Medical Sonography — What Is a Sonographer? — https://www.sdms.org/resources/careers/work-description American Society for Clinical Laboratory Science — Medical Laboratory Professionals Information about laboratory careers and how lab professionals support diagnosis and treatment. Link: American Society for Clinical Laboratory Science — Medical Laboratory Professionals — https://ascls.org/about-us/medical-laboratory-professionals/ MedlinePlus — Medical Tests Patient-friendly explanations of many common lab tests and why clinicians order them. Link: MedlinePlus — Medical Tests — https://medlineplus.gov/lab-tests/In Req 5, you will bring career exploration into the real world by planning a workplace visit and learning how to ask better questions.
Req 5 — Making the Most of a Workplace Visit
This requirement turns health care from a list on a page into a real place with real people. A workplace visit helps you notice details you would never get from a career website alone: the pace, the sounds, the teamwork, the tools, and the way a professional talks to patients and coworkers.
Before you visit, make a plan. Know which career you are exploring, bring a notebook, dress appropriately, and ask your parent or guardian and counselor for approval. Your goal is not to impress anyone. Your goal is to listen carefully and come away with honest observations.
Requirement 5a: Why They Chose the Career
Career choices are often more personal than Scouts expect. One professional may have been inspired by a family member’s illness. Another may have loved biology, anatomy, or engineering. Someone else may have chosen a path because they wanted direct patient contact, predictable hours, or the chance to work in emergencies.
When you ask this question, listen for turning points. Did a volunteer experience matter? Did a mentor encourage them? Did they switch careers after discovering a better fit? The answer helps you see that careers are shaped by values and interests, not just pay or prestige.
Requirement 5b: What They Like Most
The answer to this question reveals what makes the work meaningful. Some professionals love solving difficult cases. Others love helping patients through scary moments. A therapist may enjoy watching progress over time. A lab or imaging professional may love accuracy, technology, and helping the team reach the right diagnosis.
Try to notice whether the person’s favorite part matches what you would enjoy. A career that sounds impressive may not fit your personality, while a less famous role may suit you perfectly.
Requirement 5c: Biggest Challenges
Every health care job comes with pressure. Challenges may include long hours, emotional situations, difficult paperwork, shift work, emergencies, or the responsibility of avoiding mistakes when patients are counting on you.
This question matters because it keeps career exploration honest. A strong answer shows both the rewards and the hard parts.
Requirement 5d: Tools and Instruments
Tools tell you a lot about a career. A pharmacist may rely on dispensing systems, medication databases, and barcode checks. A podiatrist may use imaging, exam tools, and casting materials. A sonographer depends on ultrasound equipment. An EMT uses airway tools, stretchers, and monitors.
Look for both physical tools and digital tools. In health care, computers, imaging systems, electronic records, and decision-support software are often just as important as stethoscopes or syringes.
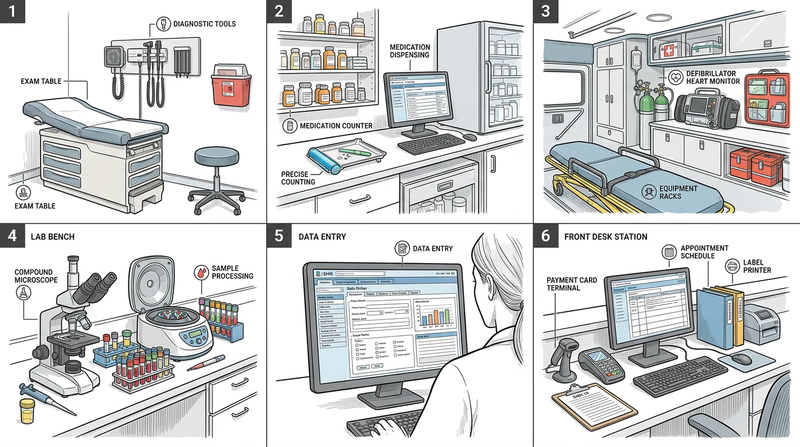
What to Observe During Your Visit
Watch for these details while you are there- Work setting: hospital, clinic, ambulance, lab, pharmacy, school, or private office
- People interaction: how the professional talks to patients, families, and coworkers
- Tools and technology: machines, protective gear, records systems, or medical supplies
- Pace of the job: steady, rushed, appointment-based, or unpredictable
- Teamwork: who else works closely with this professional
Requirement 5e: Most Surprising Aspect
This answer often gives the most memorable insight. A professional may say the biggest surprise was how much of the job involves communication, paperwork, teaching, or teamwork instead of just science. Someone else may say the surprise was how emotionally intense the work can be.
A good surprise answer helps you move past stereotypes. For example, a pharmacist may spend more time counseling people than counting pills. A psychologist may spend a lot of time on careful assessment and documentation, not just conversation.
Requirement 5f: Continuing Education
Finishing school does not mean learning stops. Many health care professionals must complete continuing education to renew licenses or certifications. That may include formal classes, online courses, conferences, skills refreshers, or proof of ongoing clinical practice.
This requirement shows an important truth about health care: the science keeps changing. New medicines appear. Guidelines are updated. Technology improves. Ethical and legal rules shift. Good professionals keep up.
Turning the Visit Into a Strong Report
After your visit, organize your notes while the details are still fresh. You do not need a perfect essay, but you should be ready to tell your counselor:
- who you visited
- where they worked
- what you learned from each of the six discussion points
- whether the career seems more or less interesting to you now
In Req 1 through Req 4, you compared careers on paper. Here, you are adding real-world evidence.
ExploreHealthCareers.org Career profiles and planning ideas that can help you prepare better questions before your workplace visit. Link: ExploreHealthCareers.org — https://explorehealthcareers.org/ U.S. Bureau of Labor Statistics — Occupational Outlook Handbook A useful place to review day-to-day duties, work environments, and required training before you visit a professional. Link: U.S. Bureau of Labor Statistics — Occupational Outlook Handbook — https://www.bls.gov/ooh/Next, you will shift from careers to ethics by exploring one of medicine’s oldest and most important ideas: the Physician’s Oath.
Req 6 — The Physician's Oath
Before a patient ever trusts a doctor with a diagnosis, surgery, or painful personal question, there has to be something deeper than job training. There has to be an ethical promise. The Physician’s Oath is one of medicine’s oldest symbols of that promise.
When people talk about the Physician’s Oath, they usually mean the Hippocratic Oath, a tradition that reaches back to ancient Greece and the physician Hippocrates. The exact words have changed many times over the centuries, and different medical schools may use different versions today. But the big ideas remain powerful.
What the Oath Means
The Physician’s Oath is a public statement that medicine is not just a technical job. It is a moral responsibility. A physician is promising to use knowledge and skill for the benefit of patients, not for selfish reasons.
Several ideas are usually at the center:
- Help the patient. The doctor’s first duty is the well-being of the patient.
- Avoid harm. This is often linked to the phrase “First, do no harm,” even though those exact words are not the full oath.
- Respect privacy. Patients share personal details because they trust that their information will be protected.
- Practice with honesty and humility. Good physicians know their limits, keep learning, and seek help when needed.
- Treat patients with dignity. A patient is a person, not a problem to solve.
Why the Oath Still Matters Today
Modern medicine is far more complex than ancient medicine. Doctors use advanced imaging, genetic tests, AI-assisted tools, electronic records, and treatments that earlier generations could barely imagine. But all that technology raises an important question: just because we can do something, does that mean we should?
That is where medical ethics matters. The Physician’s Oath reminds doctors that science must stay connected to compassion, fairness, and respect.
🎬 Video: The Hippocratic Oath — CBS Sunday Morning — https://www.youtube.com/watch?v=iMiJDSbxLWE
How to Explain It to Your Counselor
A strong answer does not need to quote an oath word for word. Instead, explain what you think it means in plain language. You might say that the oath is a doctor’s promise to put patients first, act ethically, protect trust, and use medical knowledge responsibly.
You can also connect it to other careers in this badge. Even though this requirement names the Physician’s Oath, the same ethical ideas matter to nurses, pharmacists, therapists, technicians, and emergency responders. In health care, skill without ethics is dangerous.
Ideas to Include in Your Discussion
Use these points to build your own explanation- Why patients need trust: people may share private, scary, or embarrassing information
- Why ethics matters: health care choices can deeply affect a person’s body, future, and family
- Why humility matters: a good clinician keeps learning and does not pretend to know everything
- Why respect matters: every patient deserves dignity, even when stressed, frightened, or difficult
A Real-World Example
Imagine a doctor treating a patient who is confused, scared, and unsure whether to agree to a risky procedure. The ethical job is not just to push for the fastest answer. The doctor should explain the choices clearly, answer questions honestly, listen carefully, and recommend what seems best for the patient.
That is the spirit of the oath. It is not only about avoiding obvious harm. It is about combining knowledge with conscience.
American Medical Association — Code of Medical Ethics Overview An overview of the ethical principles physicians use to guide modern medical practice. Link: American Medical Association — Code of Medical Ethics Overview — https://code-medical-ethics.ama-assn.org/ PBS — The Hippocratic Oath Today A readable look at how the Hippocratic Oath has changed over time and why it still matters. Link: PBS — The Hippocratic Oath Today — https://www.pbs.org/wgbh/nova/article/hippocratic-oath-today/In Req 7, you will build on this idea of trust by looking at confidentiality and the privacy law known as HIPAA.
Req 7 — Confidentiality and HIPAA
A patient will not always tell the truth if they do not feel safe. If someone thinks their medical information will be shared carelessly, they may hide symptoms, skip questions, or avoid getting help at all. That is why confidentiality is not just a courtesy in health care. It is part of good care.
What Confidentiality Means
Confidentiality means health care professionals protect private patient information and share it only with the people who truly need it for treatment, payment, health care operations, or other legally allowed reasons. It helps build trust between patients and the people caring for them.
Confidential information can include:
- a diagnosis or test result
- medicines a person takes
- mental health history
- family medical history
- insurance information
- details from a visit, even the fact that a visit happened
If patients trust their information will be respected, they are more likely to be honest. That honesty helps the care team make better decisions.
What HIPAA Is
HIPAA stands for the Health Insurance Portability and Accountability Act. It is a U.S. law passed in 1996. For this requirement, the most important part is that HIPAA helps protect certain health information and sets rules for how covered health care organizations and related businesses handle it.
HIPAA does not mean health information can never be shared. It means there are rules. Information can usually be shared for legitimate care purposes, but not gossip, curiosity, or convenience.
What HIPAA Looks Like in Real Life
- A nurse should not discuss a patient’s condition where unrelated people can easily overhear.
- A receptionist should verify who is asking for information before sharing it.
- A worker should log out of a computer instead of leaving a medical record open.
- A clinician should only look at records needed for their job.
Those habits are part of privacy, even when nobody says the word HIPAA out loud.
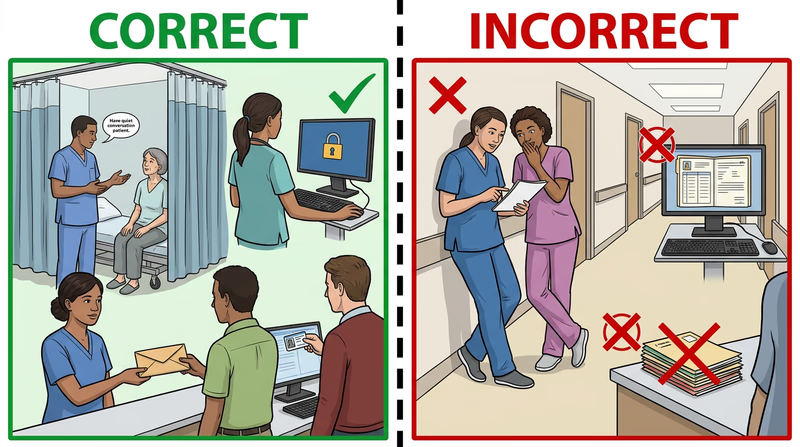
🎬 Video: 5 Scenarios of Maintaining Patient Confidentiality — Etactics — https://www.youtube.com/watch?v=8kNlqc7H8pY
Confidentiality Is Bigger Than a Law
HIPAA matters, but the idea of confidentiality is even broader. Good health care professionals respect privacy because it is the ethical thing to do, not only because they could get in trouble for breaking the rules.
This connects directly to Req 6. The Physician’s Oath is about trust and ethics. Confidentiality is one of the clearest ways that trust shows up in daily practice.
A Simple Way to Explain HIPAA
Use this structure with your counselor- What it is: a U.S. law that protects certain health information
- Why it matters: patients need privacy to trust their providers
- What it does: limits who can access or share protected information
- What it does not mean: it does not stop appropriate sharing among professionals involved in care
Everyday Examples You Can Use
A strong counselor discussion often includes examples. Here are a few:
- If a provider tells a friend about a patient’s diagnosis just because it is interesting, that breaks confidentiality.
- If a doctor sends test results to another specialist involved in the same patient’s care, that is usually allowed because it supports treatment.
- If a worker opens a family member’s chart out of curiosity, that can violate privacy rules even if they never say anything out loud.
These examples show that privacy is about both sharing and access.
U.S. Department of Health & Human Services — Health Information Privacy The federal government's main HIPAA privacy information hub, with consumer-friendly explanations and guidance. Link: U.S. Department of Health & Human Services — Health Information Privacy — https://www.hhs.gov/hipaa/index.html MedlinePlus — Personal Health Records Helpful background on health records, privacy, and how patients manage their own medical information. Link: MedlinePlus — Personal Health Records — https://medlineplus.gov/personalhealthrecords.htmlNext, you will examine how new discoveries and medical breakthroughs can change the way patients are diagnosed, treated, and cared for.
Req 8 — Recent Medical Breakthroughs
A medical breakthrough is exciting only if it helps real patients. New ideas appear in headlines all the time, but the most important question is not “Is this cool?” It is “How could this change what happens to a patient in a clinic, ambulance, hospital, or recovery program?”
One strong recent example is the growing use of artificial intelligence tools to help doctors analyze medical images and other health data. These tools do not replace health care professionals, but they may help teams spot patterns faster, catch problems earlier, and choose treatments more accurately.
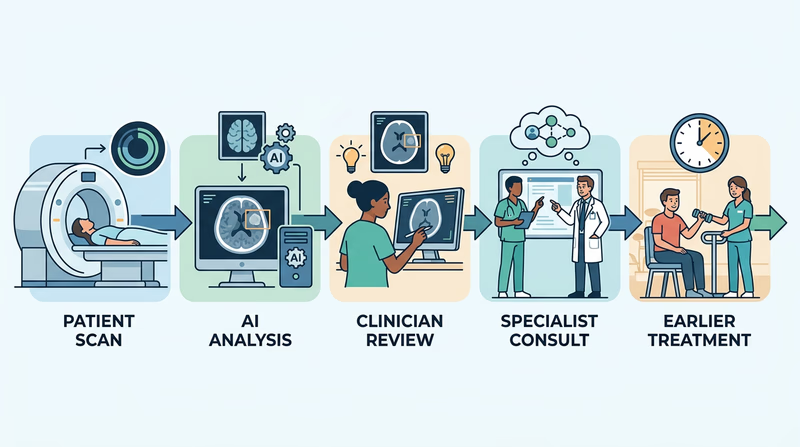
Example Breakthrough: AI-Supported Diagnosis
Imagine a child with a rare brain tumor or a patient with an X-ray, CT scan, or pathology slide that is difficult to interpret. An AI system can be trained on large numbers of past cases and then help identify patterns that might be hard for a human to notice quickly. The clinician still makes the final decision, but the tool can act like a powerful second set of eyes.
Researchers are studying AI tools for many parts of health care, including:
- analyzing scans and images
- matching patients to treatments
- predicting which patients may need faster attention
- helping organize clinical information so teams can act sooner
How This Could Affect Patient Care
Faster Answers
If a tool helps identify a serious condition sooner, treatment can begin earlier. In health care, time matters. A faster diagnosis may mean less suffering, fewer complications, or a better chance of recovery.
More Accurate Decisions
AI systems may help reduce missed details, especially in data-heavy settings. That does not mean they are perfect. It means they may support the human expert by highlighting findings worth a second look.
Better Access to Expertise
Not every clinic or hospital has a rare-disease specialist on site. If well-designed tools help local teams recognize unusual cases, patients may get referred more quickly to the right experts.
🎬 Video: High-tech hospital uses artificial intelligence in patient care — NBC News — https://www.youtube.com/watch?v=qetKUFDDF4A
Important Limits and Concerns
A medical advancement can help patients and still raise hard questions.
Technology Is Not the Same as Judgment
A doctor, nurse, or technologist still has to decide whether a suggestion makes sense for a real person. Good patient care includes context, communication, and ethics. A computer cannot replace informed consent, empathy, or professional responsibility.
Bias and Fairness Matter
If an AI tool is trained mostly on one type of patient population, it may work less well for others. That can create unfair care. New tools have to be tested carefully.
Privacy Matters Too
New technology often depends on large amounts of patient data. That connects directly to Req 7. Innovation must protect confidentiality and use health information responsibly.
How to Evaluate a Medical Breakthrough
Use these questions with any news story you choose- What problem is it trying to solve?
- How could it help patients directly?
- What risks or limits still exist?
- Who needs training to use it safely?
- How might privacy, fairness, or cost affect its success?
Other Good Topics You Could Choose Instead
You do not have to use AI for your counselor discussion. Other recent topics could include:
- gene editing and personalized medicine
- new vaccines or cancer therapies
- wearable devices that monitor patients remotely
- blood tests that help detect disease earlier
- improved prosthetics or robotic surgery systems
The best topic is one you can explain clearly. Choose something recent enough to feel current, but specific enough that you can describe how it changes patient care.
National Institutes of Health — Research News Current medical research news from NIH that can help you find a recent advancement to discuss with your counselor. Link: National Institutes of Health — Research News — https://www.nih.gov/news-events/news-releases U.S. Food and Drug Administration — Medical Devices Information about how new medical devices and technologies are reviewed and used in patient care. Link: U.S. Food and Drug Administration — Medical Devices — https://www.fda.gov/medical-devicesYour last requirement takes you into service. Instead of only studying health care, you will step into your community and help at a real health-related event or facility.
Req 9 — Volunteer in Health Care
This requirement is where the badge stops being only about careers and starts being about service. Health care is not just a collection of jobs. It is a commitment to helping people. Even a short volunteer experience can teach you how much preparation, teamwork, and respect go into serving a community well.
Finding the Right Opportunity
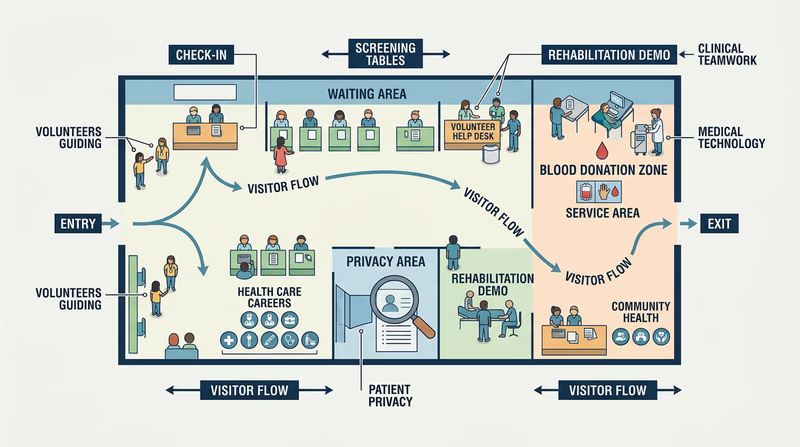
Look for events or facilities where volunteers are welcomed and where your role will be age-appropriate. Good examples include community health fairs, blood drives, vaccination clinics, hospital volunteer programs for teens, nursing home activity support, adaptive sports events, public health outreach events, and wellness screenings.
The best opportunity is not necessarily the most dramatic one. A simple job done well — greeting families, helping people find the right table, restocking supplies, setting up chairs, or guiding visitors — can still teach you a lot about how health care events operate.
Before You Volunteer
Handle the basics first- Get approval: parent or guardian first, then your counselor
- Confirm the role: know exactly what volunteers are allowed to do
- Ask about dress and arrival time: professionalism matters
- Bring a notebook: write down observations after the event, not during busy moments
- Respect privacy: never share personal patient information afterward
What to Watch For
While you serve, pay attention to more than your own task. Notice how the event is organized.
- Who greets people first?
- How is traffic or patient flow managed?
- What safety or privacy rules are obvious?
- Which professionals are present?
- How do volunteers support the professionals without getting in the way?
These observations will help you give a stronger report to your counselor later.
What You Might Learn
A volunteer experience can teach lessons that are easy to miss in a classroom:
Health Care Depends on Teamwork
Even small events require planning, supplies, communication, and backup plans. You may notice that volunteers, nurses, technicians, office staff, and community partners all have different jobs but one shared goal.
Service Includes Respect
People who come to a blood drive or health fair may be nervous, confused, tired, or dealing with a serious personal issue. Kindness, patience, and clear directions matter.
Small Jobs Matter
A volunteer who keeps forms organized, helps with setup, or calmly directs people can make the whole event work better. In health care, details are rarely “small” for long.
Reporting Back to Your Counselor
After the event, be ready to explain:
- where you served
- what your role was
- what you observed about the event or facility
- what surprised you
- what you learned about health care work or community needs
A strong report includes both facts and reflection. For example, you might say that you expected a blood drive to be mostly about needles, but you learned how much of the process depends on check-in, privacy, snack tables, and making donors feel comfortable.
American Red Cross — Volunteer A good starting point for finding community service opportunities connected to health, blood drives, disaster care, and preparedness. Link: American Red Cross — Volunteer — https://www.redcross.org/volunteer/volunteer-opportunities.html America's Blood Centers — Find a Blood Center Find local blood centers that may host drives or volunteer-supported community events. Link: America's Blood Centers — Find a Blood Center — https://www.americasblood.org/for-donors/find-a-blood-center/You have now completed the badge requirements. The Extended Learning page will help you keep exploring health care beyond the badge itself.
Extended Learning
A. Congratulations
You have just explored one of the biggest and most varied career fields in the world. That matters because health care is not only about medicine. It is about science, ethics, service, teamwork, technology, and trust.
You may now feel more interested in one specific career, or you may simply understand the health care system better than you did before. Either outcome is a win. The best next step is to keep noticing how many different ways people help patients heal, recover, and stay healthy.
B. Deep Dive: Team-Based Care
Many people picture health care as one expert walking into a room and solving a problem alone. Real health care is almost never like that. A patient with diabetes, a foot injury, hearing loss, and anxiety may need a primary care clinician, a podiatrist, an audiologist, a dietitian, a pharmacist, a psychologist, and a medical records system that helps all of them stay coordinated.
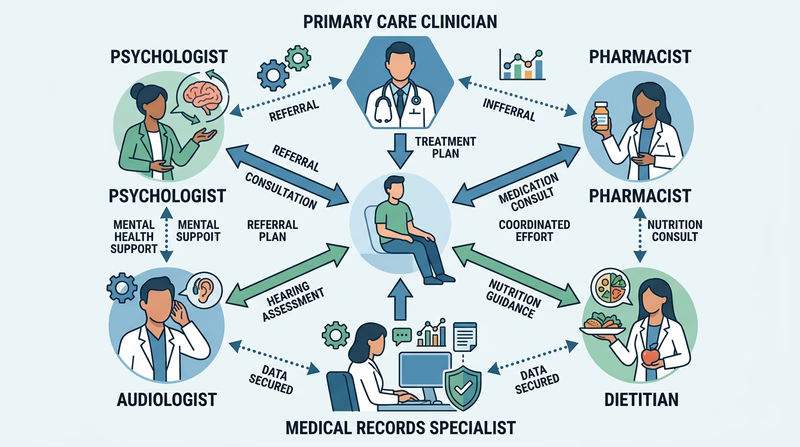
That is called team-based care. The goal is not just to bring many professionals into the same building. The goal is to make sure each professional contributes the right expertise at the right time. One person may diagnose. Another may teach. Another may monitor progress. Another may handle equipment or lab testing. Good care happens when those pieces connect.
Team-based care also reduces the chance that a patient falls through the cracks. If everyone communicates clearly, medicines are safer, follow-up is more likely, and the patient spends less time trying to repeat the same story over and over. This is one reason electronic health records, care coordinators, and standardized communication tools matter so much.
If you are interested in leadership, team-based care is worth watching closely. Health care leaders do not just need medical knowledge. They need the ability to organize people, solve workflow problems, and keep communication strong under stress.
C. Deep Dive: Public Health and Prevention
A lot of health care happens before anyone gets seriously sick. That is the work of public health and prevention. Vaccination campaigns, nutrition education, safer road design, clean water systems, disease tracking, school screenings, and smoking prevention programs all protect communities before a patient ends up in an exam room.
This is an important shift in thinking. Clinical medicine usually focuses on one person at a time. Public health asks bigger questions: Why are asthma rates higher in one neighborhood? Why are teens missing vaccines? How can a county respond faster to an outbreak? Those questions still involve health care, but at the community scale.
Scouts can understand this especially well because Scouting already teaches preparedness and service. A blood drive, a CPR class, a sunscreen station at a summer event, or a campaign to encourage helmets and seat belts are all examples of prevention in action. They may not feel as dramatic as surgery or emergency response, but they often help more people in the long run.
If you like science plus community problem-solving, public health can be a powerful direction. It includes epidemiology, health education, emergency management, environmental health, and policy work.
D. Deep Dive: Technology, Records, and Human Judgment
Modern health care uses more technology every year. Imaging systems produce detailed scans. Wearable devices track heart rhythms and glucose. AI tools may highlight patterns in records or scans. Remote monitoring lets clinicians watch some patients from home. All of this can improve care — but only if humans use it wisely.
Technology creates three big responsibilities. First, clinicians have to understand what a tool can and cannot do. Second, health systems have to protect privacy and data security. Third, professionals have to keep the patient at the center. A monitor reading is useful, but it does not replace listening to a frightened person or noticing something that a machine missed.
This matters for almost every career in the badge. A sonographer uses high-tech equipment, but still needs patient communication skills. A pharmacist may use software to catch interactions, but still has to explain the medicine clearly. A medical records specialist may protect the flow of information that allows an entire team to work safely. Technology does not remove the human side of health care. It makes the human side even more important.
E. Real-World Experiences
Try These Next
Real experiences that can deepen your understanding of health care- Tour a training program: Ask a local community college or university whether it offers open houses for nursing, EMT, radiology, respiratory therapy, or medical laboratory programs.
- Visit a simulation lab: Some schools let visitors see mannequins, mock hospital rooms, or ambulance training spaces used to teach clinical skills.
- Attend a public health event: Health fairs, CPR classes, blood drives, and community wellness events show the prevention side of health care.
- Shadow a second profession: If you already visited one kind of professional for Req 5, compare it with a very different role, such as a pharmacist, sonographer, or physical therapist.
- Volunteer more than once: Returning to the same event type can help you notice systems, teamwork, and patient communication more clearly.