
Public Health Merit Badge — Complete Digital Resource Guide
https://merit-badge.university/merit-badges/public-health/guide/
Introduction & Overview
Overview
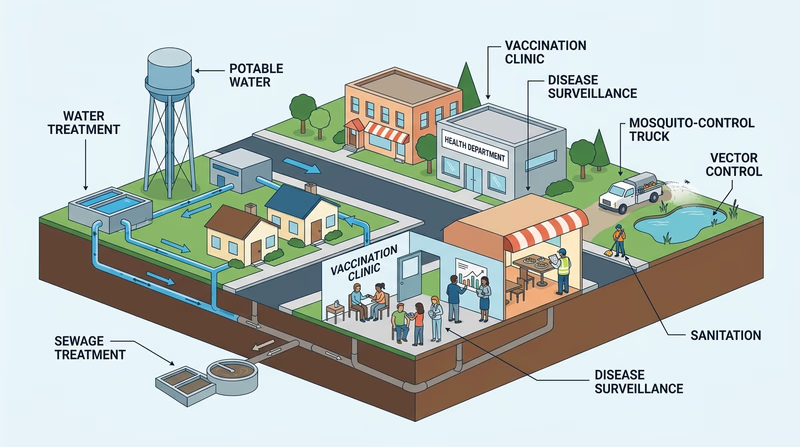
Public health is the science of helping whole communities stay healthy. It is the work behind clean drinking water, vaccination clinics, safe restaurants, mosquito control, disease tracking, and emergency response plans. Most of the time, you notice public health only when something goes wrong — but when it works well, fewer people get sick in the first place.
This badge shows you that health is bigger than one doctor’s office or one patient. Public health asks bigger questions: How do we stop disease from spreading? How do we make food and water safer? How do communities respond to disasters and outbreaks? As a Scout, you already practice many public health habits when you wash your hands, cook safely, treat water at camp, and help your unit stay prepared.
Then and Now
Then
Modern public health grew out of a simple observation: disease spreads through systems, not just through unlucky individuals. In the 1800s, cities were crowded, sewage often flowed into streets or rivers, and outbreaks of cholera, typhoid, and tuberculosis killed huge numbers of people. One of the most famous breakthroughs came in 1854, when Dr. John Snow mapped cholera cases in London and connected them to a contaminated water pump. He did not cure cholera with medicine. He helped stop it by changing the environment.
As cities learned more, they built sewers, inspected food, regulated waste disposal, and promoted hygiene. Pasteurization made milk safer. Mosquito control reduced diseases like yellow fever and malaria. Vaccines changed the story of diseases that once killed or disabled millions of children.
Now
Today, public health combines old-fashioned prevention with modern tools. Health agencies track outbreaks with lab testing and data systems. Water plants monitor contamination in real time. Epidemiologists study patterns of illness. Public information officers explain risks clearly during storms, heat waves, and disease outbreaks. Community programs focus on air quality, mental health, substance misuse, lead exposure, and other risks that affect daily life.
Public health still depends on basic habits — clean hands, safe food, good sanitation, vaccinations, and honest reporting when people get sick. The difference is scale. Instead of protecting one person at a time, public health aims to lower risk for everyone.
Get Ready!
This badge asks you to think like an investigator. You will compare diseases, study prevention, look at local systems, and see how public health decisions affect homes, camps, schools, and whole communities. Bring your curiosity — and pay attention to the hidden systems around you.
Kinds of Public Health
Infectious Disease Control
This part of public health focuses on germs and how they spread. It includes tracking outbreaks, finding sources of infection, promoting vaccination, and teaching people how to reduce exposure. Requirement 1 starts here because understanding transmission is the foundation for the rest of the badge.
Environmental Health
Air pollution, unsafe water, lead, noise, and poor waste disposal can harm people even when no virus or bacteria is involved. Environmental health professionals test, inspect, regulate, and educate so these hazards do less damage.
Food Safety
A meal can bring people together — or send a whole group home sick. Public health workers inspect kitchens, monitor outbreaks, and teach safe food handling so germs do not multiply and spread.
Emergency Preparedness
Public health agencies do much more than respond to disease. They help communities prepare for floods, tornadoes, wildfires, chemical spills, and other disasters. They plan shelters, sanitation, cleanup, communication, and recovery.
Community Health Education
A lot of prevention depends on people understanding risk. Public health workers teach families about vaccinations, safer homes, healthier habits, and where to get help. Good information is a public health tool.
Next Steps
You are about to start with the most important building block: how disease spreads, how prevention works, and why public health looks at patterns instead of isolated cases.
Req 1 — How Disease Spreads
This requirement gives you the language of public health. You will define the field, trace how infections and other hazards reach people, and organize diseases by type, transmission, prevention, and treatment. Instead of memorizing facts one by one, look for patterns.
- Start with the source: Where does the disease or hazard come from?
- Look at transmission: How does it move from place to place or person to person?
- Think about prevention: What breaks that chain?
- Notice the difference: Some diseases come from germs, some from toxins, and some from environmental exposure.
Requirement 1a
Public health is the work of protecting and improving the health of groups of people rather than treating one patient at a time. A doctor may treat one person with food poisoning. Public health asks why several people got sick, whether the source was a restaurant, and how to stop more cases.
Public health uses prevention as its main tool. That includes safe water, vaccination, sanitation, health education, food inspections, mosquito control, emergency planning, and data tracking. The goal is not only to cure illness after it happens. The goal is to make illness less likely in the first place.
A helpful way to remember it is this: medicine treats the person in front of you; public health protects the people around them too. That is why public health workers pay attention to patterns, environments, and shared risks.
American Public Health Association — What Is Public Health? A leading professional organization for the field. Use it to see how public health connects prevention, policy, education, and community action. Link: American Public Health Association — What Is Public Health? — https://www.apha.org/Requirement 1b
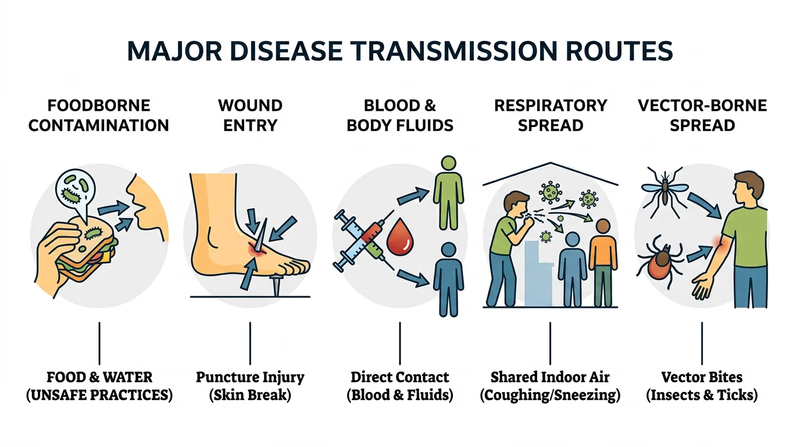
These seven examples show several different transmission routes.
| Disease or condition | Usually contracted by |
|---|---|
| E. coli | Eating or drinking something contaminated with certain strains of the bacteria, or through poor hand hygiene after contact with feces or contaminated surfaces |
| Tetanus | Bacteria entering the body through a wound, especially dirty punctures or injuries involving contaminated soil or dust |
| AIDS | AIDS is the late stage of HIV infection. HIV spreads through specific body fluids such as blood, semen, vaginal fluids, rectal fluids, or breast milk |
| Encephalitis | This is brain inflammation with several possible causes; some forms follow viral infections and some are spread by mosquito or tick bites |
| Salmonellosis | Eating contaminated food, especially undercooked poultry or eggs, unwashed produce, or through contact with infected animals or their droppings |
| Lyme disease | Being bitten by an infected blacklegged tick |
| COVID-19 | Breathing in virus-containing droplets or aerosols, especially in close indoor contact with an infected person |
When you explain these to your counselor, do not stop at the disease name. Be precise about the route: foodborne, bloodborne, wound-related, vector-borne, or respiratory. That is what makes prevention strategies make sense.
Requirement 1c
For this part, the key verbs are contracted and possibly prevented. The strongest way to prepare is to treat each disease as a two-part question:
- How does it reach the body?
- What action lowers that risk?
You only need to choose four, but studying the full list helps you pick a balanced set instead of four diseases that all spread the same way.
| Disease or condition | Usually contracted by | Possible prevention to explain |
|---|---|---|
| Gonorrhea | Sexual contact with an infected person | Safer sexual-health practices, testing, early treatment |
| West Nile virus | Bite from an infected mosquito | Repellent, long sleeves, draining standing water, screens |
| Botulism | Eating food containing botulinum toxin, especially improperly canned or preserved food | Safe canning, proper food storage, avoiding bulging or spoiled containers |
| Influenza | Respiratory droplets or aerosols from an infected person | Annual vaccination, handwashing, staying home when sick, covering coughs |
| Syphilis | Sexual contact with an infected person; sometimes passed from pregnant parent to baby | Safer sexual-health practices, testing, prompt treatment |
| Hepatitis | Varies by type: some spread through contaminated food or water, others through blood or body fluids | Vaccination for some types, handwashing, safe food and water, avoiding blood exposure |
| Emphysema | Usually develops after long-term exposure to tobacco smoke or other lung irritants | Do not smoke or vape, avoid secondhand smoke and harmful dusts or fumes |
| Meningitis | Varies by type: some spread through respiratory droplets or close contact | Vaccination for some types, handwashing, avoiding close exposure when someone is ill |
| Herpes | Direct contact with infected skin, saliva, or sexual contact depending on type | Avoid direct contact during active outbreaks, safer sexual-health practices |
| Lead poisoning | Swallowing or breathing in lead from paint dust, contaminated soil, water, or certain products | Test older homes, control dust, wash hands, avoid known lead sources |
A strong way to choose your four
Pick diseases that let you show different routes of transmission and prevention- Pick one vector-borne example: West Nile virus is the clearest one.
- Pick one food or toxin example: Botulism works well.
- Pick one respiratory or close-contact example: Influenza or meningitis.
- Pick one environmental or chronic exposure example: Lead poisoning or emphysema.
Requirement 1d
This part is broader than 1c. Now you are not picking four. You are comparing all 10 using the same four lenses:
- type or form
- possible vectors
- prevention or reduced spread
- available treatments
A chart works especially well here because the requirement is asking for side-by-side analysis.
| Disease or condition | Type or form | Possible vectors | Prevention or reduced spread | Available treatments |
|---|---|---|---|---|
| Gonorrhea | Bacterial | None in the insect sense | Safer sexual-health practices, testing, prompt care of partners | Antibiotics |
| West Nile virus | Viral | Mosquitoes | Repellent, drain standing water, protective clothing, screens | Supportive care; severe cases need medical treatment |
| Botulism | Toxin produced by bacteria | None | Safe food preservation, safe canning, refrigeration when needed | Urgent medical care, antitoxin, breathing support in severe cases |
| Influenza | Viral | None | Annual vaccination, handwashing, respiratory hygiene, staying home when sick | Rest, fluids, supportive care, antiviral medicine for some cases |
| Syphilis | Bacterial | None | Safer sexual-health practices, testing, prompt treatment | Antibiotics |
| Hepatitis | Viral in the most common forms discussed here | None | Vaccination for some types, safe food and water, avoiding blood or body-fluid exposure | Depends on type; supportive care or antiviral treatment for some forms |
| Emphysema | Chronic lung disease; environmental or exposure-related | None | Avoid smoking, vaping, secondhand smoke, and chronic lung irritants | Inhaled medicines, oxygen for some patients, pulmonary rehab, stopping exposure |
| Meningitis | Often viral or bacterial | None | Vaccination for some forms, handwashing, limiting close exposure, rapid medical evaluation | Depends on cause; bacterial meningitis needs urgent antibiotics, viral cases often need supportive care |
| Herpes | Viral | None | Avoid direct contact during outbreaks, safer sexual-health practices | Antiviral medicines can help control symptoms and reduce spread |
| Lead poisoning | Environmental toxic exposure | None | Remove lead sources, wet-clean dust, test older homes or water, wash hands | Remove exposure; medical follow-up and sometimes chelation therapy |
What the word “vector” means here
The requirement asks for possible vectors for transmission, but only a few items on this list truly use vectors. West Nile virus is the clearest example because mosquitoes carry it from host to host. Most of the others spread by contact, air, food, blood, or environmental exposure instead.
What makes this comparison useful
This chart helps you explain why prevention changes from one disease to the next. Vaccination helps with influenza and some hepatitis or meningitis risks, but it does nothing for lead poisoning. Mosquito control matters for West Nile virus, but not for gonorrhea. Antibiotics help bacterial diseases, but not viral ones.
CDC — Clean Hands A useful reminder that many infectious-disease prevention strategies begin with handwashing and other basic hygiene habits. Link: CDC — Clean Hands — https://www.cdc.gov/clean-hands/about/index.html CDC — Tick Bite Prevention Helpful for comparing true vector-borne transmission with diseases that spread by other routes. Link: CDC — Tick Bite Prevention — https://www.cdc.gov/ticks/prevention/index.htmlYou now have the core idea behind the badge: diseases and health hazards follow patterns. In the next requirement, you will look at one of public health’s strongest prevention tools.
Req 2 — Immunization Basics
This requirement covers three linked ideas: what immunization is, which diseases vaccines help prevent, and where vaccines are not currently available. Public health is strongest when people understand both the power and the limits of immunization.
Requirement 2a
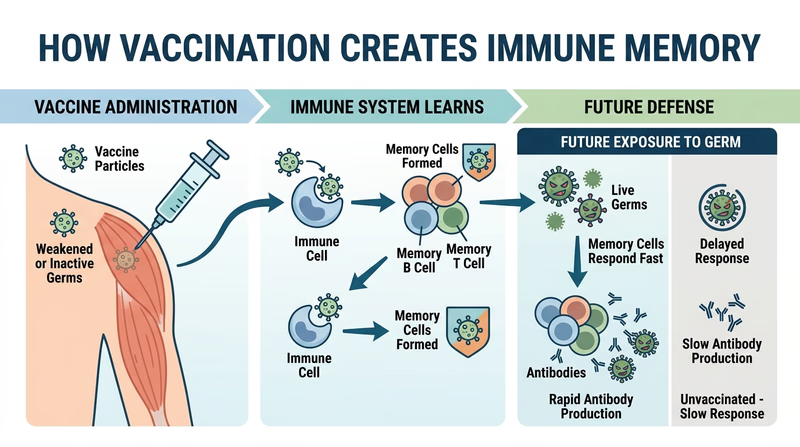
Immunization is the process of helping the body build protection against a disease, usually through vaccination. A vaccine trains your immune system to recognize a germ or part of a germ so your body can respond faster and more effectively later.
The important idea is preparation. Your immune system has “memory.” After immunization, it may recognize the threat before the real infection can do major damage. That does not always mean a person will never get sick. It often means they are less likely to get seriously sick, be hospitalized, or spread the disease widely.
Immunization also protects communities. When many people are protected, a germ has fewer easy paths to move through a school, troop, neighborhood, or family.
Requirement 2b
For this discussion, focus on the pattern rather than trying to sound perfect from memory. Your counselor wants to know that you understand how vaccine schedules work.
Young children are commonly immunized against several serious diseases early in life. Examples often discussed in childhood vaccine schedules include measles, mumps, rubella, polio, diphtheria, tetanus, pertussis, chickenpox, hepatitis B, and certain bacterial infections such as Hib or pneumococcal disease. Your counselor may want current local recommendations, so use an up-to-date source.
Two examples of diseases for which people may need periodic reimmunization or booster protection include tetanus and COVID-19, depending on current guidance and age or risk group. The classic annual immunization is influenza.
Requirement 2c
This part matters because vaccines are powerful, but they do not exist for everything. Some conditions in Requirement 1 are not prevented by routine vaccination at all. Lead poisoning is an exposure problem, not an infectious disease. Emphysema is usually prevented by avoiding tobacco smoke and harmful inhaled irritants. Lyme disease prevention mainly depends on avoiding tick bites. Salmonellosis prevention depends heavily on safe food handling.
Even when no vaccine is available, public health still has tools. Those tools include sanitation, better food safety, pest control, protective equipment, safer behaviors, testing, early treatment, and education.
When there is no vaccine
Ask what public health uses instead- Environmental controls: remove lead, improve ventilation, improve sanitation
- Behavior changes: safer handling of food, safer sex practices, handwashing
- Vector control: reduce mosquitoes and ticks
- Early detection: testing, reporting, and contact tracing when needed
- Treatment and follow-up: reduce complications and further spread
🎬 Video: How do vaccines help babies fight infections? | How Vaccines Work — Centers for Disease Control and Prevention (CDC) — https://www.youtube.com/watch?v=k7DGeWlKu0Q
Public health cannot vaccinate away every problem, so the next requirement moves to another major defense: safe water and sanitation.
Req 3 — Safe Water and Clean Gear
A single bottle of stream water can look crystal clear and still carry bacteria, viruses, or parasites. At camp, water safety is public health in miniature: one bad source or one sloppy cleanup routine can turn a fun weekend into a campwide outbreak of stomach illness.
Why safe drinking water matters
Unsafe water spreads disease because it can carry germs from human waste, animal waste, dirty containers, or contaminated ground. When people drink that water, use it to wash dishes, or mix it into food, the germs get a new path into the body.
That is why public health puts so much effort into treatment plants, sewer systems, testing, and education. In the backcountry, you become the treatment system. You are the last barrier between a water source and your body.
Two ways to make water safe at camp
You need to demonstrate two methods, so it helps to understand the strengths of each.
Boiling
Boiling is one of the most dependable field methods. Bring water to a rolling boil, then follow current backcountry guidance for how long to keep it there, especially if you are at high elevation. Boiling kills disease-causing organisms through heat.
Best for: uncertain water sources, cold-weather trips, and situations where you can use a stove or fire safely.
Filtration or purification treatment
Portable filters remove many harmful organisms, while chemical treatments or purifier systems work by killing or inactivating them. Some tools do one job better than the other, so Scouts should know what their device is designed to handle.
Best for: lighter packs, faster processing, and situations where fuel is limited.
What to show in your demonstration
Make your counselor discussion practical- Source choice: Start with the cleanest water you can find.
- Method steps: Explain each step in the correct order.
- Limitations: Say what your method does well and what it may not handle.
- Storage: Keep treated water in a clean container so it does not get re-contaminated.

Washing dishes and utensils safely
Clean dishes are part of disease prevention. If plates, pots, cups, or utensils stay greasy, damp, or dirty, germs can keep growing and spread to the next meal.
At home, dishwashers and hot running water do much of the work. At camp, you need a system.
A simple camp dishwashing flow
- Scrape food scraps first. Less food left on dishes means less organic material for germs.
- Wash in hot, soapy water. This removes grease and visible dirt.
- Rinse in clean water. Soap left behind is unpleasant and can interfere with sanitation steps.
- Sanitize when appropriate. Follow the guidance your unit and counselor use for camp sanitation.
- Air-dry completely. Towels can spread contamination if they are dirty. Air-drying is usually safer than wiping everything dry with the same cloth.
Keeping gear sanitary
Store dry dishes off the ground and protected from insects, dirt, and splash. Do not stack wet cups inside each other. At home or camp, moisture plus leftover food is an invitation for microbial growth.
🎬 Video: How to Filter Water in the Backcountry || REI — REI — https://www.youtube.com/watch?v=Kb_6eXF8kVE
You have now looked at disease prevention through sanitation. Next comes another big public health strategy: controlling the animals that carry disease from place to place.
Req 4 — Vectors and Pest Control
A vector is a living organism that carries a disease-causing germ from one host to another. Mosquitoes, ticks, fleas, and some rodents are classic examples. The vector may not be the disease itself, but it can be the vehicle that moves the disease.
Why does this matter? Because controlling the vector often lowers disease even when you cannot eliminate the germ completely. You may not be able to remove West Nile virus from nature, but you can reduce standing water where mosquitoes breed.
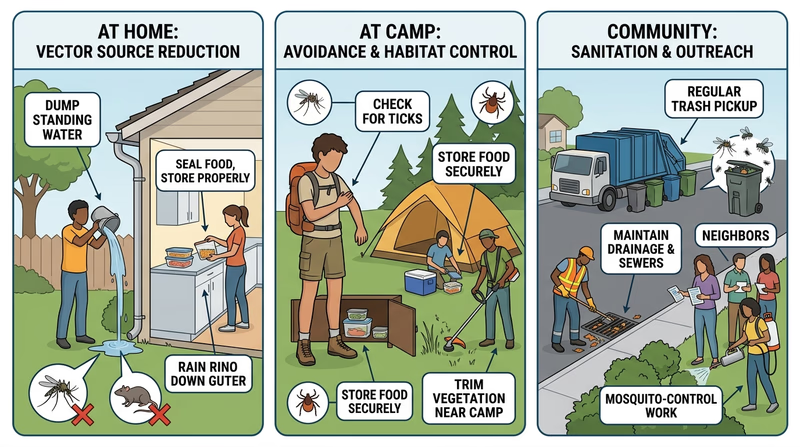
Home and camp control: what individuals can do
Many vector problems start with habits and local conditions.
Mosquitoes
Mosquitoes breed in standing water. Individuals can dump water from buckets, flowerpots, tarps, old tires, and clogged gutters. At camp, empty containers, avoid leaving puddle traps around the site, and wear long sleeves or repellent when mosquitoes are active.
Ticks
Individuals can reduce tick risk by staying on trails, wearing long pants, using repellent as directed, and checking skin and clothing after outdoor activities. Campsites with tall grass and brush increase tick exposure.
Rodents
Mice and rats are attracted by food, trash, water, and shelter. At home and camp, store food in sealed containers, clean up crumbs, remove trash promptly, and block small entry points where rodents can get inside.
Simple vector control that Scouts can do
Small actions can lower risk fast- Dump standing water around camp or home.
- Store food tightly so rodents cannot reach it.
- Keep sleeping and cooking areas clean to reduce pests.
- Wear protective clothing and check for ticks after outdoor activity.
- Report infestations early before they become larger problems.
What requires community-level action
Some vector problems are too large for one family or one patrol to solve alone.
Mosquito control across an entire town may require drainage work, seasonal monitoring, larvicide programs, public education, and coordinated treatment in high-risk areas. Rat control in a city may depend on trash systems, building maintenance, sewer conditions, and neighborhood-wide enforcement. Lead-up work such as abandoned-lot cleanup or storm-drain maintenance also reduces vector habitat.
This is a key public health lesson: some health risks are personal, but many are shared. If one house is spotless but the whole neighborhood has unmanaged trash and standing water, the problem can still spread.
Why vector control is important
Vector control prevents disease, lowers medical costs, protects outdoor recreation, and keeps outbreaks smaller. It also protects people who may not be able to protect themselves easily, including young children, older adults, and people with weaker immune systems.
After learning how communities control risk, you are ready to compare two real-world public health systems and choose which one to investigate.
Req 5 — Choose Your Field Investigation
You must choose exactly one option from this requirement. Both options show public health at work in the real world, but they focus on different systems and different risks.
Your Options
- Req 5a — Waste and Wastewater Systems: Visit a wastewater treatment plant or solid-waste operation and learn how a community handles sewage or trash safely. You will see how public health protects water, soil, and people by controlling waste before it spreads disease.
- Req 5b — Food Safety in Action: Visit a restaurant, cafeteria, or similar food service facility and study how food is stored, handled, cooked, and monitored. You will learn how public health prevents contamination before a meal reaches a plate.
How to Choose
Choosing your investigation
Think about what you want to observe and discuss- Best fit if you like systems and infrastructure: Choose 5a. You will see large-scale public health work that most people never notice.
- Best fit if you like kitchens, practical routines, and daily habits: Choose 5b. You will study contamination control in a setting most people use every day.
- Time and access: A cafeteria or restaurant visit may be easier to arrange locally, while a treatment plant tour may need more planning.
- What you will gain: 5a teaches how communities manage waste and protect shared resources. 5b teaches how food safety depends on temperature, storage, sanitation, and attention to detail.
| Option | Main focus | What you observe | What you gain |
|---|---|---|---|
| 5a | Waste systems | Disposal, treatment, sanitation, environmental protection | A bigger-picture view of how cities prevent contamination |
| 5b | Food safety | Kitchen workflow, storage, temperatures, contamination prevention | A practical understanding of how public health protects meals every day |
You only choose one path, but both lead to the same public health lesson: prevention depends on systems people follow consistently.
Req 5a — Waste and Wastewater Systems
This option is about hidden systems. Most people flush, throw something away, and stop thinking about it. Public health workers cannot do that. They have to make sure sewage and trash are collected, separated, treated, and disposed of in ways that do not contaminate water, soil, food, or air.
Requirement 5a1
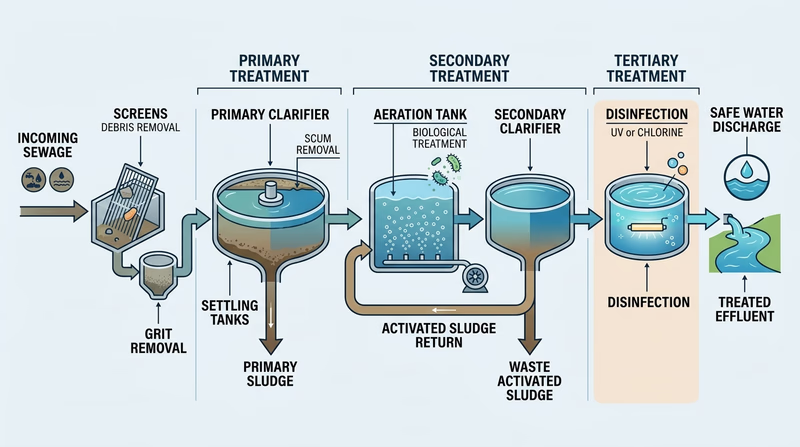
If you visit a wastewater treatment plant, watch for stages such as screening, settling, biological treatment, disinfection, and careful release or reuse. Each step removes something different: large debris, solids, organic waste, or harmful microbes.
If you visit a solid-waste operation, look for sorting, containment, compaction, recycling, hazardous-waste separation, and methods that keep leaking material from reaching soil or groundwater. Modern landfills are engineered systems, not just giant holes in the ground.
A strong answer to your counselor explains the process in order and ties each step back to public health. Ask yourself: What problem would happen if this step were skipped?
Questions to ask during the visit
These help you turn observations into a better explanation- What are the first safety checks when waste arrives?
- How does the facility separate dangerous material from ordinary waste?
- What happens to liquids, odors, or runoff?
- How does the facility keep workers and the public safe?
- What laws or inspections does the facility have to follow?
Requirement 5a2
Do not just retell the tour in order. Pull out the most important ideas.
- What surprised you?
- Which safety step seemed most important?
- What part of the process depends on trained workers making good decisions?
- What would happen in your community if this facility shut down for a week?
Those questions turn a visit into a public health discussion instead of a travel report.
Requirement 5a3
In the wilderness, you do not have pipes, pumps, or engineered landfills. That means your patrol has to use outdoor ethics and sanitation skills to keep the environment — and other people — safe.
Human waste should be handled according to local rules and Leave No Trace guidance. In some places that means catholes; in others, it means pack-it-out systems or designated toilets. Trash should never be buried unless local rules explicitly allow a specific practice, because animals dig it up and weather exposes it again. Food scraps, grease, and wash water can attract animals and contaminate campsites.
The main public health idea is simple: keep waste away from water, camps, food areas, and wildlife.
EPA — Facts and Figures about Materials, Waste and Recycling Useful context for understanding how large the solid-waste challenge is and why safe management matters. Link: EPA — Facts and Figures about Materials, Waste and Recycling — https://www.epa.gov/facts-and-figures-about-materials-waste-and-recyclingIf this option is not the one you plan to do, compare it with the food-service option next. If it is your choice, the next page still helps you see how public health works in another everyday system.
Req 5b — Food Safety in Action
This option shows how public health works minute by minute. In a kitchen, safety depends on many small decisions: where food is stored, how hands are washed, whether raw meat touches ready-to-eat food, and whether someone checks temperatures instead of guessing.
Requirement 5b1
Preparation and workflow
Watch how food moves through the kitchen. Safe facilities separate raw and cooked foods, keep work surfaces clean, and avoid confusing workflows where one mistake can spread contamination.
Handling and hygiene
Food handlers protect meals by washing hands, using clean tools, avoiding bare-hand contact when appropriate, and staying home when sick. Good habits matter because bacteria do not need a dramatic mistake to spread.
Storage and contamination control
Cold foods should stay cold, hot foods should stay hot, and storage should keep drips, spills, and raw products from contaminating other items. Labels, dates, and organized shelving are public health tools, not just kitchen neatness.
What to notice during your visit
Look for signs that contamination is being prevented on purpose- Separate areas for raw and ready-to-eat foods
- Handwashing stations that are easy to reach and actually used
- Covered, labeled storage in refrigerators and dry goods areas
- Clean thermometers and sanitation tools ready to use
- Managers or staff checking routines instead of assuming everything is fine
Requirement 5b2
Conditions that help microorganisms grow
Microorganisms grow best when they have moisture, nutrients, the right temperature, and enough time. Many foods provide all four. That is why cooked rice, meat, dairy, soups, sauces, and cut produce can become risky if they sit too long.
Preventing growth and spread
The best prevention methods are keeping food out of unsafe temperature ranges, avoiding cross-contamination, cleaning surfaces, washing hands, chilling leftovers quickly, and using safe storage times.
Killing harmful microorganisms
Proper cooking is one of the most important ways to kill disease-causing microbes. Heat works only if the food actually reaches the needed internal temperature, which is why guessing by color or “looks done” is not enough.

Requirement 5b3
A thermometer replaces guessing with evidence. You cannot tell a safe internal temperature just by looking at meat, casseroles, or leftovers. Color, texture, and steam can fool you.
Thermometers also matter for refrigerators, freezers, hot-holding equipment, and dish sanitation systems. Public health depends on measurements because harmful microorganisms grow when food stays too warm for too long.
🎬 Video: The Importance of Cooking to a Safe Internal Temperature and How to Use a Food Thermometer — USDAFoodSafety — https://www.youtube.com/watch?v=-2KkV2yFiN0
Requirement 5b4
When you report back, focus on what the facility does to prevent a problem before anyone gets sick. That is the public health mindset.
Good discussion points include:
- the most important contamination-control step you saw
- one routine that looked small but mattered a lot
- how staff balanced speed with safety
- what could go wrong if the system broke down for one shift
You have now studied two real-world prevention systems. Next, the guide broadens out to other public health hazards in air, water, noise, and substance use.
Req 6 — Pollution and Substance Risks
This requirement looks at health dangers that do not all spread the same way. Some come from polluted environments. Some come from substances people choose to use. Public health studies both because both can harm individuals, families, and whole communities.
Requirement 6a
Air pollution can irritate the eyes and lungs, worsen asthma, damage the heart and blood vessels, and make outdoor activity less safe on poor-air-quality days. Smoke from wildfires, traffic emissions, and industrial pollutants are all examples.
Water pollution can introduce chemicals, sewage, or harmful organisms into drinking or recreation water. That can lead to infections, poisoning, or long-term health effects depending on the contaminant.
Noise pollution may not seem as dramatic, but repeated high noise exposure can damage hearing, increase stress, disturb sleep, and make concentration harder. Once hearing is damaged, it often does not come back.
Requirement 6b
Tobacco harms nearly every part of the body. It damages the lungs, raises the risk of cancer, harms the heart and blood vessels, and exposes other people through secondhand smoke or aerosol.
Alcohol abuse can affect judgment, coordination, memory, and decision-making right away. Over time, it can damage the liver, heart, brain, and relationships. For teens, alcohol also increases the risk of injuries, dangerous choices, and impaired driving situations.
Drug abuse can injure the brain and body, increase overdose risk, damage trust, and make school, family, and mental health challenges harder.
Requirement 6c
Illegal drugs can cause poisoning, addiction, dangerous behavior, and overdose. Prescription drugs can also become dangerous when misused — for example, taken in the wrong amount, used without a prescription, mixed with other substances, or taken for the feeling instead of the medical purpose.
A key public health point is that a drug’s legal status is not the same thing as its safety in every situation. A medicine can help when used correctly and become dangerous when misused.
Prescription-drug misuse is especially risky because people may wrongly assume, “It came from a pharmacy, so it must be safe.” Safe use depends on dose, timing, purpose, storage, and the person it was prescribed for.
Patterns to mention in your discussion
Show that you understand both immediate and long-term harm- Immediate risks: impaired judgment, poisoning, overdose, injury
- Long-term risks: organ damage, addiction, lung injury, brain effects
- Community effects: family stress, crashes, healthcare burden, lost learning time
- Prevention: education, safe storage, refusal skills, supportive adults, treatment resources
Public health is not only about risk factors. It is also about institutions that track problems and respond to them. The next pages turn to health agencies and how they protect a community.
Req 7a — Choose Your Agency Research Path
You must choose exactly one option from this requirement. Both paths teach you how a health agency works, but one does it through an in-person visit and the other through careful research online.
Your Options
- Req 7a1 — Visit a Public Health Agency: Meet public health work face to face. You may see offices, lab or field programs, inspection systems, emergency planning, or community-health services in action. This option helps you understand the people and systems behind the agency.
- Req 7a2 — Investigate an Agency Website: Study what the agency publishes online — current alerts, statistics, programs, resources, inspections, and emergency guidance. This option helps you understand how agencies communicate with the public and organize information.
How to Choose
Choosing between a visit and a website study
Both satisfy the requirement, but they teach different things- Best for seeing the human side of the work: Choose 7a1. You can ask questions and notice things that never appear on a webpage.
- Best for flexible scheduling: Choose 7a2. You can do detailed research even if an in-person visit is hard to arrange.
- Best for current examples and public alerts: Choose 7a2. Agency websites often show real-time priorities.
- What you will gain: 7a1 gives you direct experience with professionals and procedures. 7a2 builds research skills and helps you interpret how agencies serve the public through information.
You are not just completing a visit or browsing a site. You are preparing to explain how a real health agency responds to disease, mortality, and disasters.
Req 7a1 — Visit a Public Health Agency
If you visit an agency, pay attention to what it actually does for the community each day. Public health agencies are not just office buildings. They may manage inspections, disease reporting, maternal and child health programs, environmental testing, vaccination efforts, emergency planning, or public messaging.
What to look for
Notice the connection between information and action. Where does the agency get health data? How does it decide what to warn the public about? Which programs are focused on prevention, and which are focused on response after a problem is already underway?
Good questions to ask
- What are this agency’s biggest public health concerns right now?
- How does the agency learn about disease outbreaks or environmental hazards?
- Which services are aimed at prevention?
- How does the agency work with schools, hospitals, emergency managers, or the public?
- What does the agency do during a disaster?
A strong visit report should describe not only where you went, but how that agency protects people who may never meet the staff personally.
NACCHO — Local Health Departments A national organization focused on county and city health departments. Helpful for understanding what local public health agencies do. Link: NACCHO — Local Health Departments — https://www.naccho.org/The website option covers the same broad topic from a different angle. Reading it will help even if you plan to complete the visit option.
Req 7a2 — Investigate an Agency Website
A good health agency website is a public health tool. It tells people what risks are current, what services are available, where to get help, and how to prepare. When you explore the site, do not skim randomly. Hunt for evidence of what the agency actually does.
What to explore
Look for pages related to disease reporting, vaccinations, environmental health, restaurant inspections, emergency preparedness, data dashboards, seasonal alerts, and public advisories. Those sections show what the agency considers important and how it communicates with the public.
Questions to answer from the website
- What are the agency’s main divisions or responsibilities?
- What current issues or alerts are highlighted?
- What data or reports does it share with the public?
- What services can residents use directly?
- How does it guide people during emergencies or outbreaks?
A smart way to study the website
Collect examples you can bring into Requirement 7b- Save three useful pages: alerts, services, or dashboards
- Write down one statistic or report title the agency publishes
- Find one outbreak-related page and one disaster-related page
- Notice how the site serves different audiences such as parents, schools, travelers, or healthcare workers
Whether you visit in person or study a website, the next requirement asks the bigger question: how does an agency respond to death, disease, outbreaks, and disasters in a real community?
Req 7b — How Agencies Protect Communities
This requirement asks you to connect what you observed in 7a to bigger community outcomes. Public health agencies do not just publish facts. They try to lower death rates, reduce disease, respond to outbreaks, and help communities recover from disasters.
Requirement 7b1
Mortality means death. Morbidity means illness, injury, or the burden of disease. They overlap, but they are not the same thing. A condition can cause a lot of illness without being one of the top causes of death.
For example, a community may have heart disease or cancer among the top causes of death, while influenza, COVID-19, sexually transmitted infections, or asthma-related illness create high morbidity without leading the death list in the same way. Public health agencies need to track both.
How agencies try to reduce both
Agencies may run vaccination campaigns, tobacco-use prevention, clean-water programs, inspection programs, outreach to high-risk groups, overdose prevention work, and education about chronic disease risk factors such as diet, exercise, or blood-pressure screening.
Your job is not to solve the whole problem. Your job is to explain how the agency’s programs line up with the problems shown by the data.
A strong comparison for your counselor
Use this structure when you organize your notes- Top causes of death: list four from a reliable local source
- Top causes of illness: list four common disease burdens or reportable conditions
- Where they overlap: notice any shared risk factors
- Agency response: connect each issue to a real program, campaign, inspection effort, or public message
Requirement 7b2
During an outbreak, health agencies track cases, confirm information, identify patterns, warn the public, and coordinate with hospitals, labs, schools, and other partners. They may issue guidance on testing, isolation, vaccination, sanitation, or exposure reduction depending on the situation.
A public health agency is part detective, part communicator, and part coordinator. It does not just say, “People are sick.” It asks where the cases are coming from, who is at risk, what actions should happen next, and how to reduce spread.
Common outbreak roles
- collecting and analyzing case reports
- confirming diagnoses through labs or partners
- identifying likely sources and transmission patterns
- informing the public clearly without causing panic
- coordinating prevention steps across agencies and institutions
🎬 Video: CDC NERD Academy Student Quick Learn: How is an outbreak investigated? — Centers for Disease Control and Prevention (CDC) — https://www.youtube.com/watch?v=kYFIqTbRd2o
Requirement 7b3
After a disaster, public health problems do not end when the wind stops or the floodwater drops. Safe water may be interrupted. Food may spoil. Mold may spread. Sewage systems may fail. People may need shelter, sanitation, vaccination, medical guidance, or help understanding whether an area is safe.
Public health agencies may help with shelter sanitation, boil-water notices, food-safety guidance, debris-related health warnings, vector control after flooding, vaccination clinics, and cleanup advice for homes and community spaces.
ASTHO — State and Territorial Public Health A helpful resource for understanding how public health agencies work at the state level during everyday operations and emergencies. Link: ASTHO — State and Territorial Public Health — https://www.astho.org/You have now looked at public health as a system of prevention, response, and recovery. The last badge requirement asks you to connect that work to a real career path.
Req 8 — Explore a Public Health Career
Public health is not one job. It is a team made up of many kinds of professionals who solve different parts of the same problem. Some work in labs. Some inspect restaurants or water systems. Some study disease patterns with data. Some lead emergency response. Some teach communities how to lower risk.
Public health careers you might explore
Here are a few strong choices:
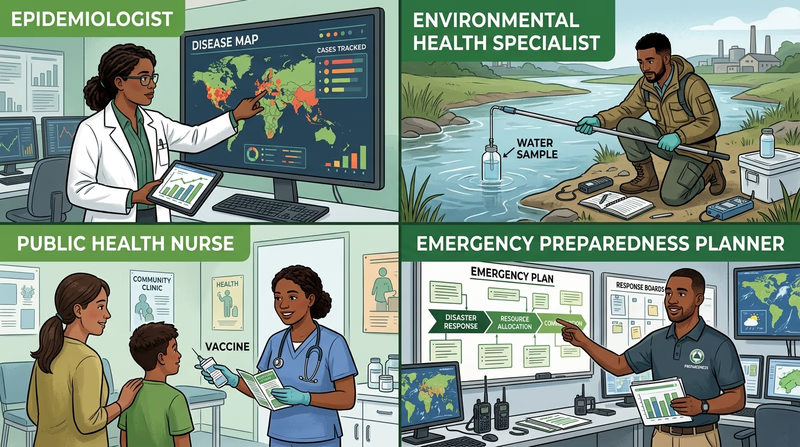
- Epidemiologist — studies patterns of disease and helps track outbreaks
- Environmental health specialist — investigates water, waste, housing, lead, and sanitation risks
- Public health nurse — connects medical care with prevention and community programs
- Health educator — helps communities understand risks and make healthier choices
- Food inspector or sanitarian — checks facilities for food-safety problems
- Emergency preparedness coordinator — plans for disasters and recovery
What to research
No matter which profession you choose, answer the same core questions.
Education
What degree is typical? Some roles start with a bachelor’s degree in biology, public health, environmental science, nursing, or a related field. Others may require graduate study, certifications, or professional licensure.
Training
What job-specific training is needed? This might include field investigation methods, lab methods, inspection training, emergency management courses, or data analysis skills.
Experience
How do people get started? Internships, volunteer work, local health-department opportunities, research assistant roles, and college field experiences can all build a path into the field.
What to bring to your counselor discussion
Show that you researched the profession like a real possibility- What the job does each day
- What education is required
- What training or certifications matter
- What experience helps someone get hired
- Why the career interests you
🎬 Video: Public Health Careers: Epidemiologist, Part 1 — Centers for Disease Control and Prevention (CDC) — https://www.youtube.com/watch?v=tYx-fO5hMA4
You have completed the badge requirements. The Extended Learning page goes beyond the minimum and shows where public health can lead next.
Extended Learning
Congratulations!
You have finished a badge that most people do not think about until a crisis happens. Now you know better. Public health is the quiet work that keeps drinking water safe, food cleaner, neighborhoods healthier, and disasters from becoming even worse. Once you start noticing those systems, you see them everywhere.
Outbreak Detective Work
One of the most fascinating parts of public health is epidemiology — the science of figuring out who is getting sick, where, when, and why. Outbreak detectives compare patterns, interview people, trace common exposures, and test whether one suspected source really fits the evidence.
That work is a lot like solving a mystery, except the goal is not just to know what happened. The goal is to stop it from happening again. If you liked the badge sections on disease spread and health agencies, epidemiology is worth a deeper look.
Designing Healthier Places
Public health is shaped by design decisions. Sidewalks, parks, storm drains, housing quality, restaurant training, lead-safe renovations, and access to clinics all affect health long before anyone ends up in a hospital.
This is one reason public health is such a wide field. Engineers, inspectors, educators, nurses, communicators, planners, and scientists all contribute. A healthier community is usually the result of many systems working together.
Public Health Communication
A good public health message is clear, calm, and useful. During a storm, disease outbreak, or heat wave, people need to know what to do next — not just what went wrong. That means public health agencies must turn science into actions ordinary people can follow.
If you enjoy writing, explaining, designing graphics, or speaking to groups, public health communication could be a strong career path. Communities need people who can explain risk without confusion or panic.
Real-World Experiences
Tour a Water or Wastewater Utility
Attend a Local Board of Health or City Meeting
Volunteer at a Community Health Event
Take CERT or Youth Preparedness Training
Shadow a Public Health Professional
Organizations
A major professional organization for public health. Its site highlights current issues, advocacy, education, and the many branches of the field.
Organization: American Public Health Association (APHA) — https://www.apha.org/
Represents local health departments and helps explain how public health works close to home.
Organization: National Association of County and City Health Officials (NACCHO) — https://www.naccho.org/
Shows how state and territorial agencies support public health systems, emergency response, and long-term planning.
Organization: Association of State and Territorial Health Officials (ASTHO) — https://www.astho.org/
A central U.S. public health agency offering outbreak information, prevention guidance, and educational resources across many health topics.
Organization: Centers for Disease Control and Prevention (CDC) — https://www.cdc.gov/
A key source for environmental health topics such as air quality, water safety, pollution, and hazardous exposure.
Organization: Environmental Protection Agency (EPA) — https://www.epa.gov/